Our survey of adult Boston residents, conducted during the fall of 2020 asked, “If a vaccine against the coronavirus becomes available, do you plan to get vaccinated?” We found that about 1 in 5 respondents were not planning to get vaccinated: almost 9% stated they were “definitely not” planning to get vaccinated and about 12% stated they were “probably not” getting vaccinated. We examined the percentage of adult residents likely to avoid vaccination by age, gender, education, having children in the household, and race or ethnicity.
Our report, Living in Boston during COVID-19: Vaccine Hesitancy, estimated the percentage of adult residents in 25 Boston neighborhoods who were likely to say that they “probably” or “definitely” do not plan to get vaccinated to prevent infection from COVID-19. To get these rates, we calculated hesitancy rates for the population by race and ethnicity and extrapolated to neighborhoods using American Community Survey data for race and ethnicity in each neighborhood. Figure 1 shows that vaccine hesitancy rates (either definitely or probably not getting the vaccine) were highest last fall in neighborhoods with a greater concentration of Black and African American residents—Mattapan, Roxbury, Dorchester Central, and Hyde Park.
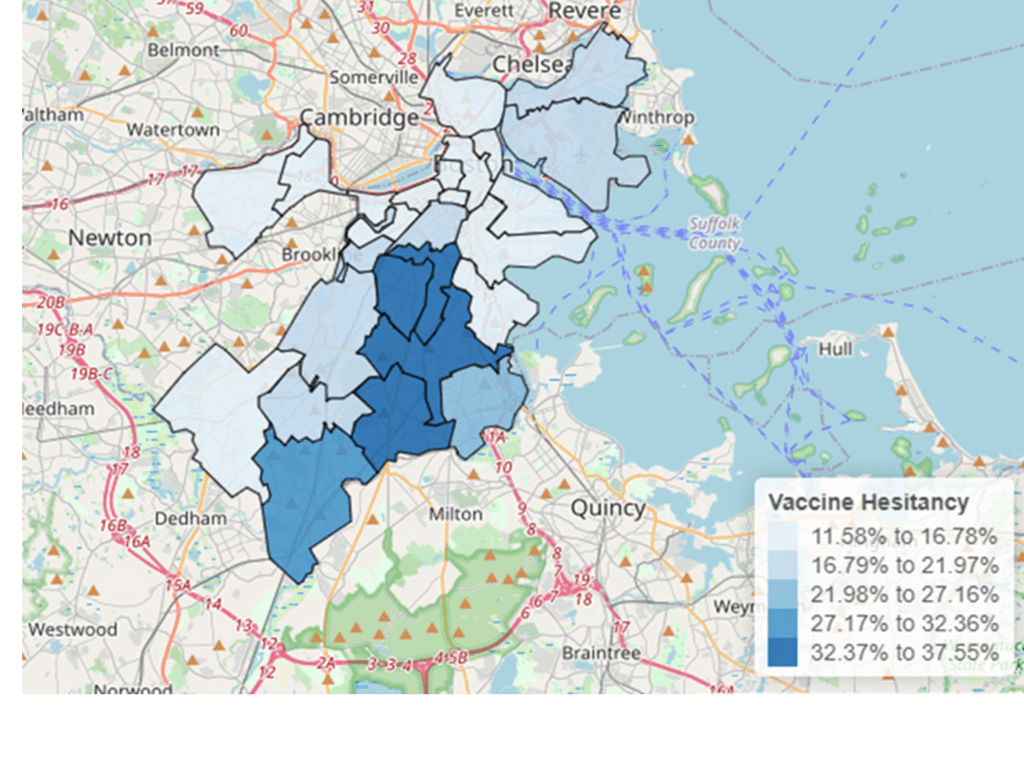
Figure 1. Percentage of respondents “Definitely not” or “Probably not” planning to get the vaccine in Boston neighborhoods extrapolated from Living in Boston during COVID-19 survey data to American Community Survey race and ethnicity data for each neighborhood
This picture of vaccine hesitancy in neighborhoods may best viewed through the lens of respondents’ personal characteristics, particularly race and ethnicity. Figure 2 shows the following:
- Almost one-half of Black respondents stated they probably or definitely were not planning to get the vaccine,
- One-quarter of Latinx respondents indicated they do not plan to get the vaccine, and
- Fewer than 1 in 10 White and Asian/Pacific Islanders probably or definitely did not plan to get vaccinated.
Reluctance to be first to get a COVID-19 vaccine is not surprising given general knowledge of past injustices in health care delivery and research.
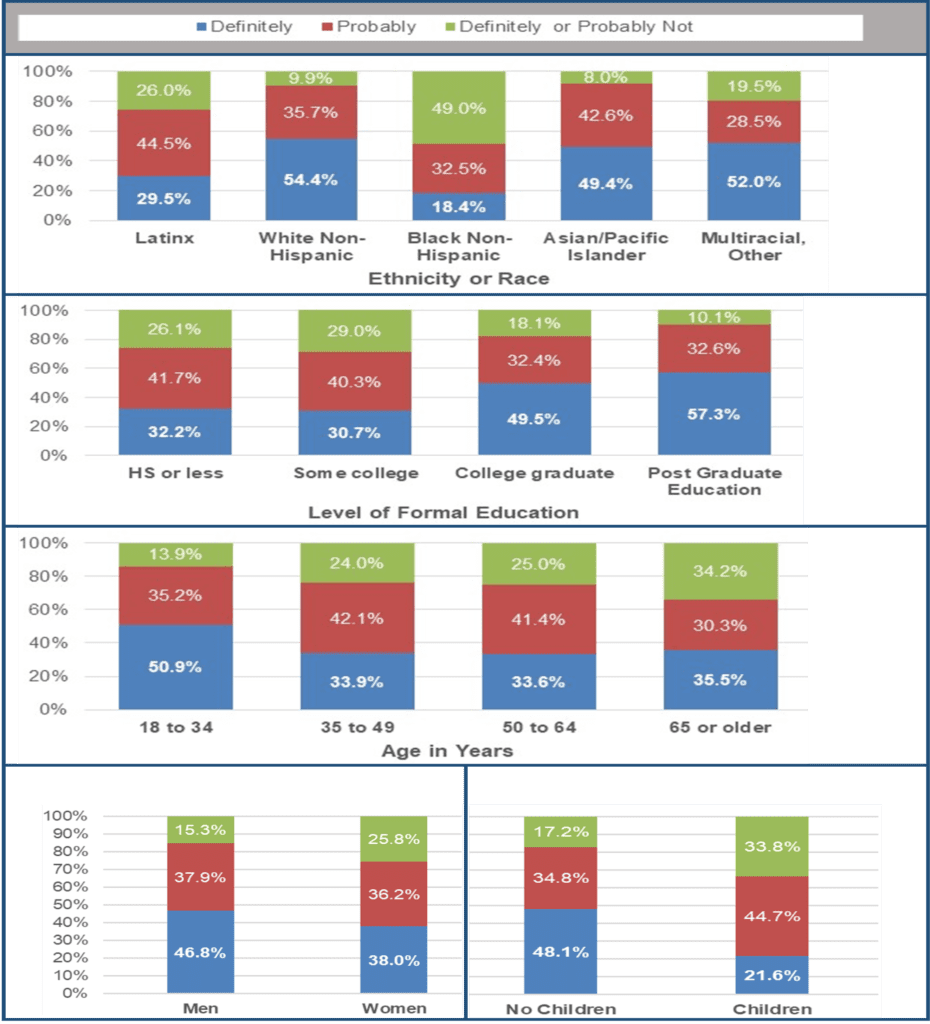
Figure 2. Personal characteristics associated with plans to get a COVID-19 vaccine
Additional findings based on respondents’ personal characteristics show that education level is associate with vaccine hesitancy—those with a college education are more likely to have definite plans to get the vaccine and respondents with a high school education or some college are less likely.
Reluctance to be the first to get a COVID-19 vaccine is not surprising given a general knowledge of past injustices in health care delivery and research. Additional findings based on respondents’ personal characteristics show that education level is associate with vaccine hesitancy—those with a college education are more likely to have definite plans to get the vaccine and respondents with a high school education or some college are less likely.
The association of age with vaccine hesitancy is complex. Younger respondents, aged from 18 to 34, clearly are enthusiastic about COVID-19 vaccination, over one half definitely plan to get the vaccine. At the same time, in older age groups there is some hesitancy, 1 in 3 respondents over age 65 have no plan to get vaccinated.
Hesitancy in planning to get a vaccine was much more prevalent among women respondents with over 1 in 4 women stating they did not plan to get a COVID-19 vaccine, compared to fewer than 1 in 6 men. People with a child in the household are less likely to plan for vaccination—1 in 3 people with a child in the household were hesitant, compared to l in 5 people without children in the household.
Conclusions
Using responses to our Living in Boston during COVID-19 follow-up survey, we provide information about which Boston residents are clearly likely to get vaccinated and those who are more likely to hesitate. This information can be used to develop personalized messages to both listen to concerns about vaccine and encourage widespread vaccination among diverse groups of Bostonians.
To prevent spread of the coronavirus, significant proportions of residents in Boston neighborhoods will need to obtain a vaccine. Figure 3 presents infection rates collected by the Boston Public Health Commission for the time period coinciding with the Living in Boston during COVID-19 survey. The urgency for vaccination is underscored by seeing the incidence of COVID-19 infection is highest in neighborhoods with many residents having some hesitancy to get vaccinated. Thus, people with the greatest need for vaccination may pass on the opportunity to build immunity in their neighborhood. As community leaders and public health agencies work to persuade people to plan to get vaccinated when offered, they can ask reluctant residents about their concerns and consider how their personal backgrounds may influence decision-making about vaccination. Some people’s reluctance may be shaped by an understanding of historical inequities in the health care system or by past injustices in health care delivery and research based on race and by general concerns about risks of vaccination.
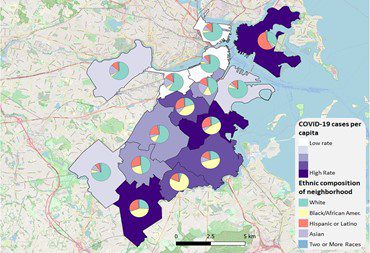
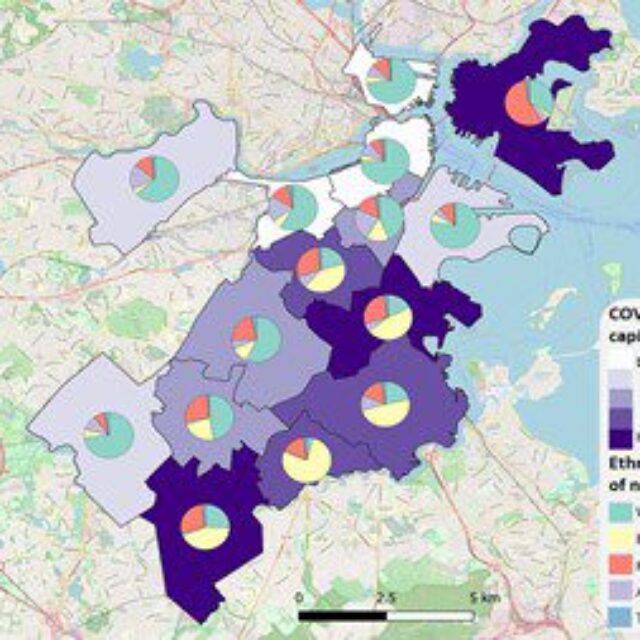
Figure 3. COVID-19 infection rates per 100,000 residents, September 17, 2020 and ethnic composition of neighborhoods from the American Community Survey
Our neighborhood-level estimates are based on survey responses from fall 2020. The COVID-19 vaccine began distribution in December 2020. As vaccination rolls out throughout the Commonwealth of Massachusetts and vaccination rates in particular neighborhoods climb, the rates of acceptance among Boston residents in communities of color may shift in a positive direction.
[1] Cases per capita rates from low to high, where low rates are about 1100 cases per 100,000 and high rates are around 4950/100,000 and the median rate for Boston is 2380 per 100,000. Weekly reports from the BPHC are here, https://bphc.org/whatwedo/infectious-diseases/Documents/Forms/AllItems.aspx
[2] https://www.mass.gov/covid-19-vaccine-in-massachusetts, accessed 5 January 2021
The content of this post is drawn from the Living in Boston during COVID survey conducted by the Boston Area Research Initiative, the Center for Survey Research at UMass Boston, and the Boston Public Health Commission. It was funded by the National Science Foundation’s Human-Environment and Geographical Sciences (HEGS) program through a grant for rapid-response research (RAPID; Award #2032384). The results presented here were part of a longer report on Vaccination Planning and Hesitancy.